Forever in Flux: The Demographics of Healthcare Workers Amidst an Uncertain Pandemic
By Anabel Moore
For most Americans, the last eighteen months of pandemic life have seemed to stretch on forever; our normal days and routines upended by quarantine requirements, travel restrictions, and on-again, off-again lockdowns. The pandemic’s initial effects in Spring of 2020 were significant: panic-buying and toilet paper hoarding, at-home workouts and dreaded Zoom calls. The following summer was marginally more hopeful, with decreased cases enabling outdoor get-togethers. However, the virus came back with renewed ferocity in the fall, forcing students to either return to school in person full-time (some wearing masks, some not) or learn completely online, opening up a schism between wealthy and low-income students. Finally, the world got the ultimate Christmas gift: vaccinations. Since then, we’ve been living in a state of “in-between” as officials juggle bipartisan desires to reopen with still lagging vaccination rates, especially in areas with a more politically conservative population.
But for one distinct group of people, the last eighteen months have been a particularly punishing slog through the depths of human suffering and resilience. While working themselves to the bone and putting their own lives at risk, roughly 9.8 million patient-facing American healthcare workers now have to manage their own decisions to be vaccinated while struggling with the moral and ethical pitfalls of caring for acutely ill unvaccinated people. These two challenges have produced stark demographic changes in an already overburdened system. The last year and half has been the ultimate stress test for this demographic dynamic, with one researcher noting that we may continue to see an even wider shift in the workforce as workers who are vaccinated and tired of caring for unvaccinated patients shift away from patient-facing work while those that are unvaccinated leave facilities with vaccination mandates.
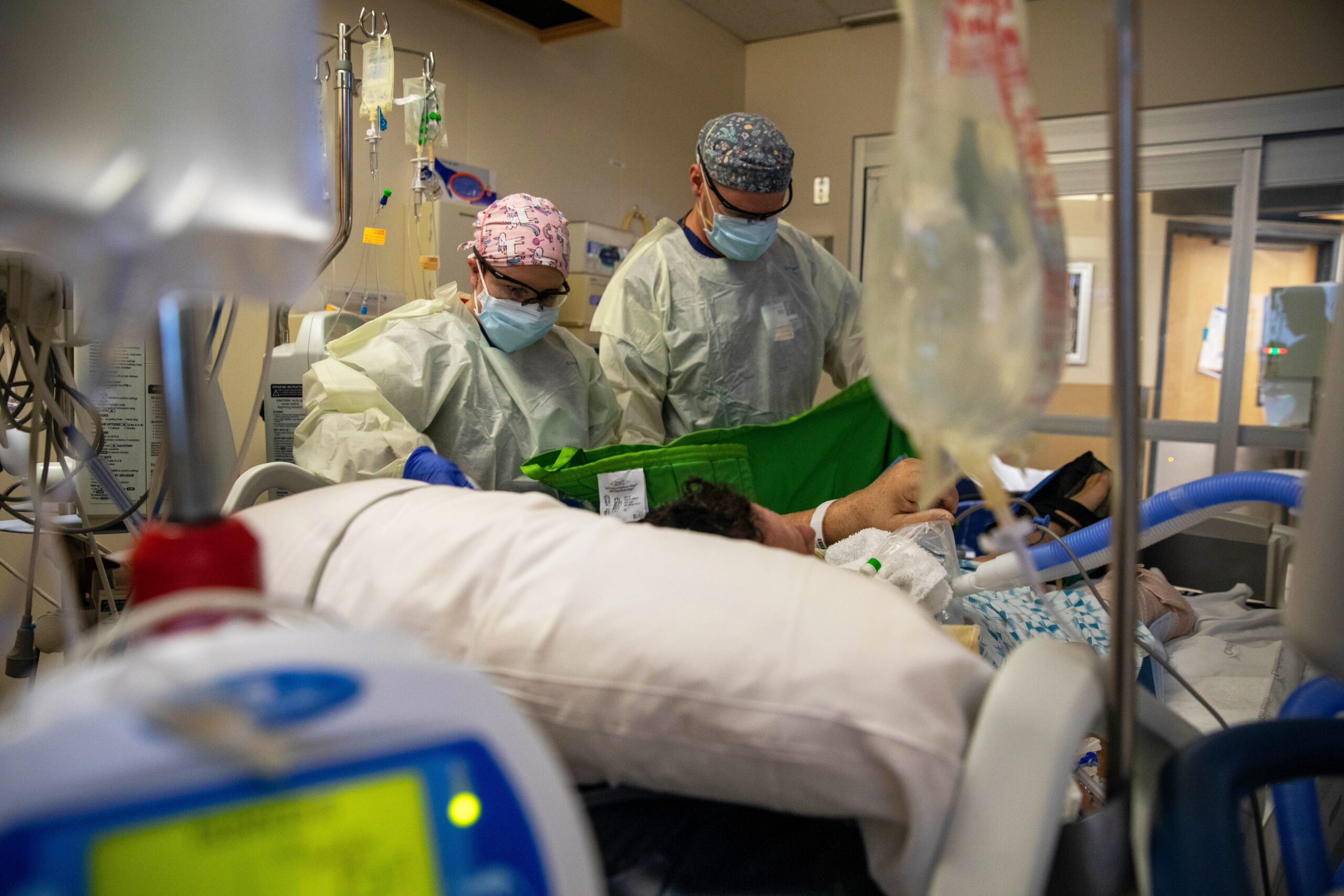
For Peyton Wilson, pandemic care was one of the first steps in her nursing career. Working as a traveling nurse on the West Coast, Wilson described her time living out of a locked-down hotel and caring for acutely ill COVID-19 patients as incredibly stressful and difficult.
“There were no breaks. We didn’t have the time or staff to take breaks, and we’d be in full gear for hours and hours. A lot of the patients didn’t get the care they would be getting now or should be getting because we were so busy and overrun and overworked. It was the bare minimum to keep these people alive, which was sad in a lot of ways. You couldn’t give the care you wanted and the care you were used to giving. It was just whatever you could do to make it work and make it through the day.”
Though the crisis of the pandemic in America isn’t as significant now as it was then, the country is now facing a crisis of polarization, in which individual decisions to be vaccinated or unvaccinated are the difference between a overwhelmed healthcare system and a stable, relatively calm hospital environment.
Dr. Ivette Motola, assistant director of the University of Miami Gordon Center for Simulation and Innovation in Medical Education, described the difference in how healthcare workers are perceived between the beginning of the pandemic and now. According to Motola, back in the spring of 2020, the public in Little Havana would hit pots at 8 PM, clapping for and cheering on their healthcare heroes.
“It felt like those were so many of the reasons you go into medicine – you really want to help people and want them to get better. That carried folks for a while. But when the backlash came, it really impacted healthcare workers and emergency physicians who were on the front lines. When there was this whole backlash that doctors are making up that people are dying from COVID when it’s not really COVID and the mis and disinformation – it’s really hard.”
There is no more representative example of the “tale of two Americas” than the current COVID-19 outlook in Miami, Florida and New Haven, Connecticut. With many COVID-19 regulations based on political ideology, Motola noted that “the politicization of this pandemic is one of the biggest travesties I can think of in a long time. It’s just been really unfortunate.” Florida, while not the state with the lowest overall vaccination rate in the country, has only 59% of its total population fully vaccinated. Additionally, Governor Ron DeSantis has for months refused to enact a statewide mask mandate, even going so far as to ban mask mandates in schools. In late summer 2021, the state of Florida saw its highest single-day positive test rate, leaving hospitals overwhelmed and having to turn even non-COVID patients away, reporting oxygen shortages and a lack of intensive care unit beds.
Conversely, the state of Connecticut has seen a markedly different COVID response: with the highest vaccination rate in the country (70.1%) and many cities still requiring mask-wearing or proof of vaccination, local hospitals are operating relatively normally, not facing the acutely overwhelming patient load that has sent hospitals into overdrive in other parts of the country.
This dichotomy exemplifies how the pandemic is no longer a crisis for many areas of the country that have taken the necessary and relevant public health precautions to protect their citizens, while it remains a substantial threat for those that haven’t. With increasing polarization surrounding the decision to be vaccinated, so too are the state of hospitals and healthcare workers. But unlike March of 2020, healthcare workers now have much more agency in regards to where – and on whom – they practice medicine.
Dr. Rohit Sangal, Assistant Professor of Emergency Medicine and Associate Medical Director of the Yale University-New Haven adult emergency department is an expert in healthcare administration during the pandemic and commented on this newfound practitioner agency.
“There are a lot of healthcare workers deciding to leave their current jobs because they don’t want to get vaccinated. Those people are going to places that have low vaccination rates where maybe those mandates don’t exist and getting a job there. People who are vaccinated go to higher vaccination areas and people who aren’t vaccinated are going to lower vaccination areas, almost to be with people who they consider to be like-minded.”
Wilson described her experience with healthcare workers and their vaccination decisions: “I’ve heard a lot of stories of workers who choose to not get the vaccine and who are fired from their jobs they’ve worked for fifteen years, and it’s causing a big divide with us. In the beginning of the pandemic, it used to be us versus the virus, and now it’s us versus each other. We aren’t banded together anymore.”
Not even the incentive of high salaries in the healthcare field is enough to fully offset these challenges, as we’ve seen in the dramatic shortage of healthcare workers. During her time early in the pandemic, Wilson explained that “the turnover rate was high. We were working long hours, and there was a lot of death, things we couldn’t control or do anything about. There’s one month on the contract, and a lot of people could not stay that month. They’d leave after a week.” This burnout, compounded by the moral conundrums of caring for unvaccinated people, has left many healthcare professionals stepping back from the clinical setting and reapplying their skill sets in more administrative or managerial roles. Sangal describes this specific group’s general mindset as: “there is something to protect people, so why would I risk myself when someone else isn’t protecting themselves?”
Throughout the course of the pandemic, broader sentiments about public health guidance have been disproportionately impacted by fake news and misinformation, ranging from early Centers for Disease Control guidance stating that masks were not helpful in preventing the spread of disease to far-right conspiracy theories hawking “miracle treatments” such as hydroxychloroquine. But when vaccinations first came out, this misinformation took a violently dramatic turn, with individuals refusing vaccination because they believed outlandish theories such as the government implanting people with tracking chips through vaccination. With the internet, social media, and far-right politicians fanning the flames of fake news, tech giants have cracked down on sources that overtly spread misinformation, issuing bans on content that doesn’t clearly lay out the facts of vaccination: that it is safe, effective, and necessary to protect our communities and get us back to the normal state of life that we so desperately desire.
“When you talk to patients and ask if they are vaccinated, ask where they get their concerns and information, you end up spending a lot of time just trying to counsel people on why their underlying beliefs aren’t true. That’s challenging,” Sangal notes.
It is likely that a portion of society will never choose to be vaccinated, regardless of incentive or even obligation, decreasing the probability that the United States will reach herd immunity. This in turn increases the likelihood that the coronavirus will become endemic, with new strains emerging and requiring vaccinations every few years. In other words, the world won’t be returning to normal anytime soon. As a consequence, it’s likely that our healthcare system will have to adapt in order to meet the changing demands of the virus.
Adaptation has been a key word in our fight against COVID-19. In an effort to prevent unnecessary contact between healthcare professionals and the larger public, many hospitals and networks devoted time and resources towards advancing their telehealth operations, a shift that “would have taken maybe five or ten years to learn that we’ve now learned in two years,” according to Sangal.
America’s healthcare infrastructure underwent a “massive stress test,” according to Sangal, who noted that “with large healthcare institutions, it’s really easy for things to fall into silos, for departments to operate independently of each other. The pandemic made us realize that we can make massive structural changes to provide care.”
Healthcare systems in particular had to move quickly to adapt to the prolonged nature of the pandemic. Sangal notes that “there is a good amount [of information available] in the world of crisis management and how organizations respond, less so in the realm of how to respond to a prolonged crisis such as the pandemic. Things like car accidents, trauma, stroke, cardiac arrest: these tend to affect a small number of patients. You have a small influx of individuals who are very sick and require a lot of your attention and emotional engagement, but there’s an end point at which their care is done. Maybe they go to the operating room, maybe you stabilize them, maybe they’re able to go home. There’s an end point.” Having co-authored a well-publicized study at Yale on the effects of group dynamics on the overall mental health and decision-making of healthcare workers, Sangal notes that “burnout [in the healthcare profession] is already really high: how does the effect of COVID compound an already burnt-out workforce?”
Motola expanded on the idea of burnout, describing the evolution of how doctors and the systems they work in perceive burnout and self-care.
“With the pandemic, being sick and not being allowed to come into work – it’s about the first time I ever heard that. We’ve had people with IV pumps going, and the idea that ‘I’m an emergency medicine doctor and I can work through everything, I can scale that mountain no matter what’ – our own health and well-being, both mental and physical, has never come first. Back when I was in training, there was awareness of trying to do fun things together, but now there’s been research done on what’s effective. Those programs existed before the pandemic, and trying to implement them during the pandemic is variable depending on the reality of what’s going on in the hospital during those peaks. You can talk about it, but is it really happening?
The results of Sangal’s study, led by Marissa King, Professor of Organizational Behavior and Professor of Public Health, shows that healthcare workers who identified with a team had decreased overall stress levels, indicating that identifying or showing solidarity with others who are in the same situation improves overall well-being. Sangal notes that “when someone really sick with COVID comes in [to Yale-New Haven Hospital], it’s really nice to see us all come together and really do our team-based care well. They come in on the ambulance, they’re requiring extra oxygen, and you can go in with no hesitation, start the IVs, stabilize the airways, and really fall back on the great clinical training that everyone has. When you get over that initial hump of oh my goodness, someone might have COVID, we fall back on that core value of good patient care.”
It is heartening to think that the good patient care, public displays of bravery by healthcare professionals, and increased prevalence of public health initiatives has inspired a new generation of healthcare workers to join the workforce. Sangal notes that “the next generation of healthcare workers certainly may have an increased sense of purpose, as they were doing this training right when the pandemic was happening. They may have decided to enter or join emergency medicine specifically for that sense of purpose of wanting to care for someone.”
Wilson added that there is no doubt that new healthcare workers are going to find a place where they are wanted and needed. “Being needed in a field you’re working in is huge, and so is feeling that support and appreciation.”
This influx of new workers will encounter a system vastly different from the one which existed prior to the pandemic. Given all of the uncertainty surrounding the virus in relation to hospital management – the massive, system-wide ramifications of public safety measures, decreased revenue and increased operational costs, PPE shortages, and most notably capacity overload– America’s healthcare system will never be the same, perhaps for the better. Well-known for its operational inefficiencies, tangled insurance setup, and crossed wires, America’s healthcare system doesn’t stack up to healthcare systems in other developed nations. According to recent data from the Commonwealth fund, before the pandemic the US spent more on healthcare as a share of the economy yet had the lowest life expectancy and highest suicide rates amongst the 11 Organization for Economic Co-Operation and Development (OECD) countries.
There is certainly immense room for our system to grow and it will inevitably face a multitude of challenges for years to come. While it is certainly perplexing that many of our healthcare workers, many of whom have years of training in the sciences, choose to reject science and decline the vaccine, advances in hospital-based organizational development and the sudden surge in those wishing to don scrubs or a white jacket are reasons for hope – indicating something good may indeed have come out of these incredibly trying and exhausting past 18 months.
Anabel Moore is a first year in Branford college. You can contact her at anabel.moore@yale.edu.